Management of Pelvic and Acetabular Fractures
The mortality associated with pelvic fractures has decreased significantly over the past 30 years, due to improvements in early patient rescue, rapid transport from the site of injury and vigorous resuscitation.
The early management of any pelvic injury includes proper resuscitation, search for other systemic injuries which may be a threat to life/ limb/ critical organ systems and damage control interventions to address such problems (eg. Tension pneumothorax, cardiac tamponade, actively bleeding injuries, intra-cranial injuries).
As the patient’s general condition is being stabilised, mechanical stability of the pelvic ring should to be assessed Clinically and radiologically. An AP radiograph of the pelvis in conjunction with the hemo-dynamic status is enough to make a decision on emergency pelvic stabilisation. A CT scan though better, may not always be possible in a
polytraumatised patient.
Classification of the pelvic injury (according to Tile) helps to differentiate the Stable (A), Partially Stable (B) and Completely Unstable (C) injuries.
A

B

C
There are other classification systems too – notably the Young and Burgess System which is a mechanistic classification depending on the nature of the initial injury.
Emergency management of the pelvic injury includes measures for external reduction of pelvic volume which leads to compression of fracture surfaces and the open venous plexuses resulting in stoppage of bleeding. This can be achieved by an external fixator, a C-clamp, pelvic binder (regular/ pneumatic). Care is taken to see that there are no fractures where the pins are inserted.
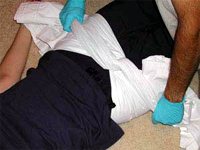
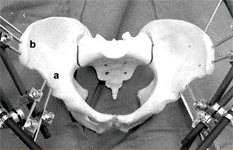

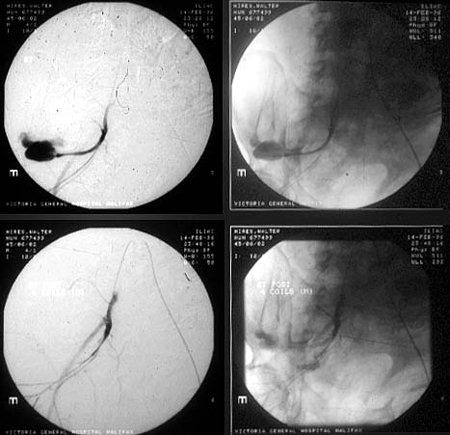
External tamponade by such measures may not be enough and a laparotomy to attend to intra- abdominal injuries and packing of the bleeders in the pelvis may be necessary. Nowadays, with advancement of interventional radiology (pin- hole surgery), embolisation of active bleeders is a minimally invasive alternative, in sselected cases.
Not all pelvic fractures require internal fixation. The fractures that need to be fixed are:
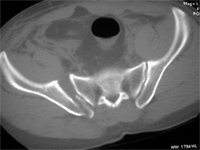
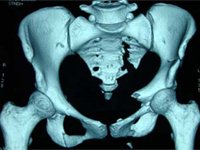
Displaced and unstable fractures/ dislocations of the posterior ring – sacrum/ilium/ sacro-iliac joint
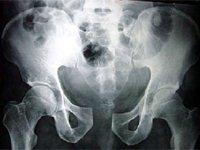
Pubic diastasis
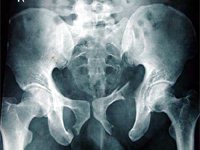
Markedly displaced fractures of the pubic ramus
It is necessary to time the definitive fixation depending on other injuries and the patient’s general status to avoid the “second hit” and multi-organ dysfunction.
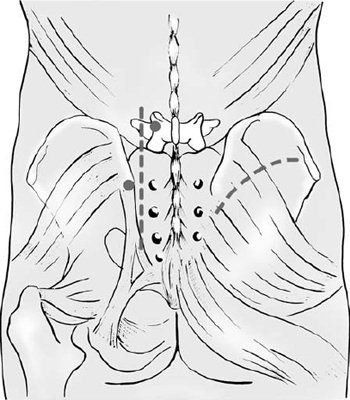
Internal Fixation
If both the anterior and posterior ring fixation is required, the posterior injury has to bee estabilised first. In some cases, posterior fixation alone is enough. However, anterior fixation alone, except in mild “open book” injuries will fail and is not recommended. Whichever segment is operated, reduction is more important and is sometimes more difficult than fixation.
Posterior Ring Fixation
Approach:
The sacro-iliac joint can be reduced by
- anterior (1st window of the ilio-inguinal approach) or
- posterior incision (lateral to posterior iliac spines)
The sacral fractures are approached by a para-median or midline incision, posteriorly. Fractures of the posterior ilium are exposed by an incision along the iliac crest.
Fixation:
Sacro-iliac Joint by percutaneous ilio- sacral screws
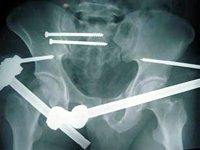
Sacrum by
- percutaneous ilio-sacral screws or
- small fragment plates
- Bridge plate between the iliac bones
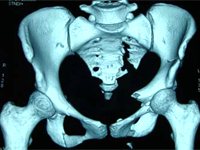
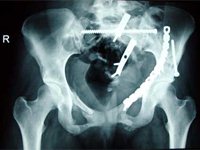
Ilium – small contourable plates along crest
Anterior Ring Fixation
Approach:
- Pfannenstiel for symphysis
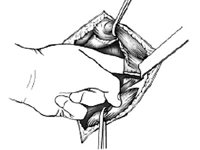
- Ilio-inguinal approach for ramus/ ilium/ pelvic brim fracture
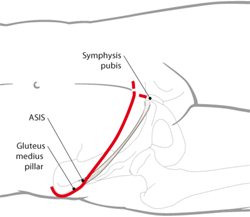
- Midline incision for symphysis injury with laparotomy
Acetabular Fractures
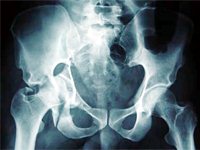
After a diagnosis of acetabular fracture is made, classification of the fracture (according to Letournel and Judet) is done with the aid of AP, obturator oblique and iliac oblique views +/- CT scan, to determine further treatment.
In acetabular fractures, minor malreductions are less tolerated than in the pelvic ring. Even so, not all fractures need surgery. The following can be treated non-operatively:
- undisplaced, stable fractures
- <20% of posterior wall involved, without displacement
- low anterior column fractures
- Transverse fractures with an adequate roof arc (Matta)
- In associated both column fractures, secondary congruence with poor general condition of patient
- Patient factors (Relative):
- old age
- general debility
- severe osteoporosis
- soft tissue injuries
Emergency Treatment:
Closed reduction of dislocations of the hip is to be undertaken as soon as possible.
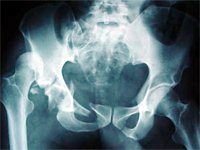
Skeletal traction is applied if the hip joint is unstable due to the fracture.
Operative treatment of acetabular fractures:
Internal fixation is almost always electively undertaken, except in post-reduction nerve palsies, open injuries or with associated pelvic fractures which require fixation.
Approaches:
- Posterior
- Kocher-Langenbeck with or without Trochanteric flip/ osteotomy
- Anterior
- Ilio-inguinal
- Ilio-femoral
- Extensile
- Extended ilio-femoral
- Maryland
- Tri-radiate
- Combined:
Fracture Patterns:
1. Simple
- Posterior wall – Kocher – Langenbeck
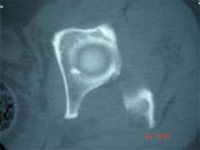
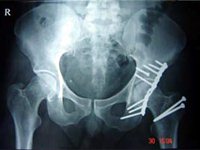
- Posterior Column – Kocher – Langenbeck
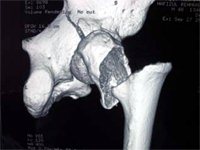
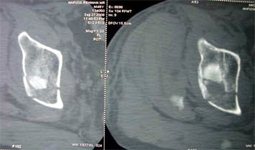
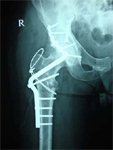
- Anterior wall – Ilio-inguinal / Ilio-femoral
- Anterior Column – Ilio – inguinal
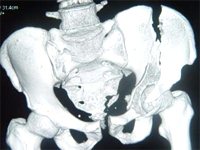
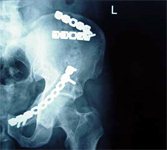
- Transverse – Kocher – Langenbeck (mostly), sometimes, Ilio-inguinal / Extensile
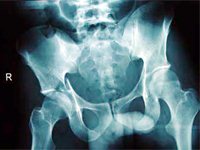
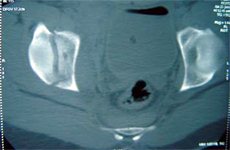
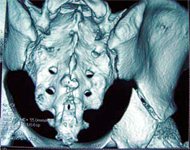
2. Associated
- Posterior wall + Posterior Column – Kocher – Langenbeck
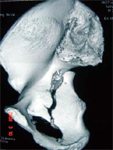
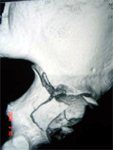
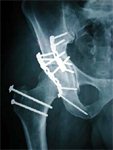
- Transverse + Posterior wall – Kocher – Langenbeck (usually), Extensile if High transverse with extended posterior wall
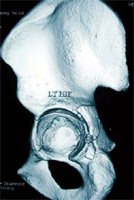
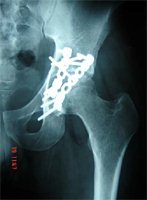
- T – fracture: Kocher – Langenbeck or Ilio-inguinal or extensile/ combined depending on the severity and differential displacement of the individual columns
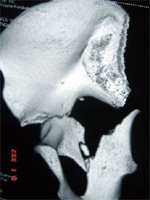
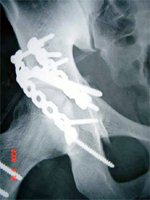
- Anterior column with Posterior Hemi-transverse: Ilio-inguinal
- Associated Both Column : Ilio-inguinal (mostly), Extensile approach
MIOT’s Approach
At MIOT Hospitals, the preferred line of management is:
Pelvic Fractures:
- Percutaneous ilio-sacral screw after open reduction by posterior approach or
- Anterior SI joint plate with plate for anterior ring, if indicated, through an ilioinguinal approach
- Symphysis plate
Acetabular fractures:
- Kocher – Langenbeck for all posterior fractures, Most transverse fractures, Transverse +posterior wall, some T-fractures
- Ilio-inguinal for all anterior fractures, most Both column fractures, anterior +hemi-transverse
- Combined for T-shaped and some Both column fractures
The frequency of combined approaches has diminished over time and single approaches are enough in most cases.
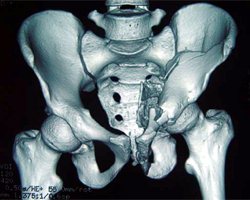
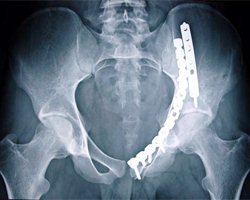

No Comments